ANNOUNCEMENT
I will be gone during Memorial Day weekend. No newsletters on Friday-Tuesday.
Lately, I've been writing a lot about Hand and Trauma because we are currently covering those topics in didactics. Also, they are my next two rotations. But in the spirit of fairness, I will try to do something else today.
What I learned today
There are two parts to this topic. Today, I’ll discuss how altered spinopelvic alignment affects total hip arthroplasty. Tomorrow, a more thorough review of spinopelvic parameters.
Spinopelvic alignment and THA
In this great primer video from Dr. Jerabek (HSS)1, he starts off by pointing out that modern hip dislocations often occur even in patients whose cup position falls within the "safe zone" (Esposito et al2, Abdel et al3).
The Lewinnek safe zone = cup inclination of 40° ± 10° and anteversion of 15° ± 10°. Previously, it was reported that staying within this zone would minimize dislocation risk for primary THA.
Unsurprisingly, now that most of our cups are positioned in this zone (hopefully), we need to dig deeper. Why are dislocations still happening?
Some plausible reasons: surgical approach, leg length / offset, femoral version, impingement, and pelvic tilt. The last three variables can be closely intertwined.
You see, pelvic tilt changes as patients move from sitting to standing and vice versa. And more posterior pelvic tilt = more functional anteversion of the acetabulum (in a normal patient).
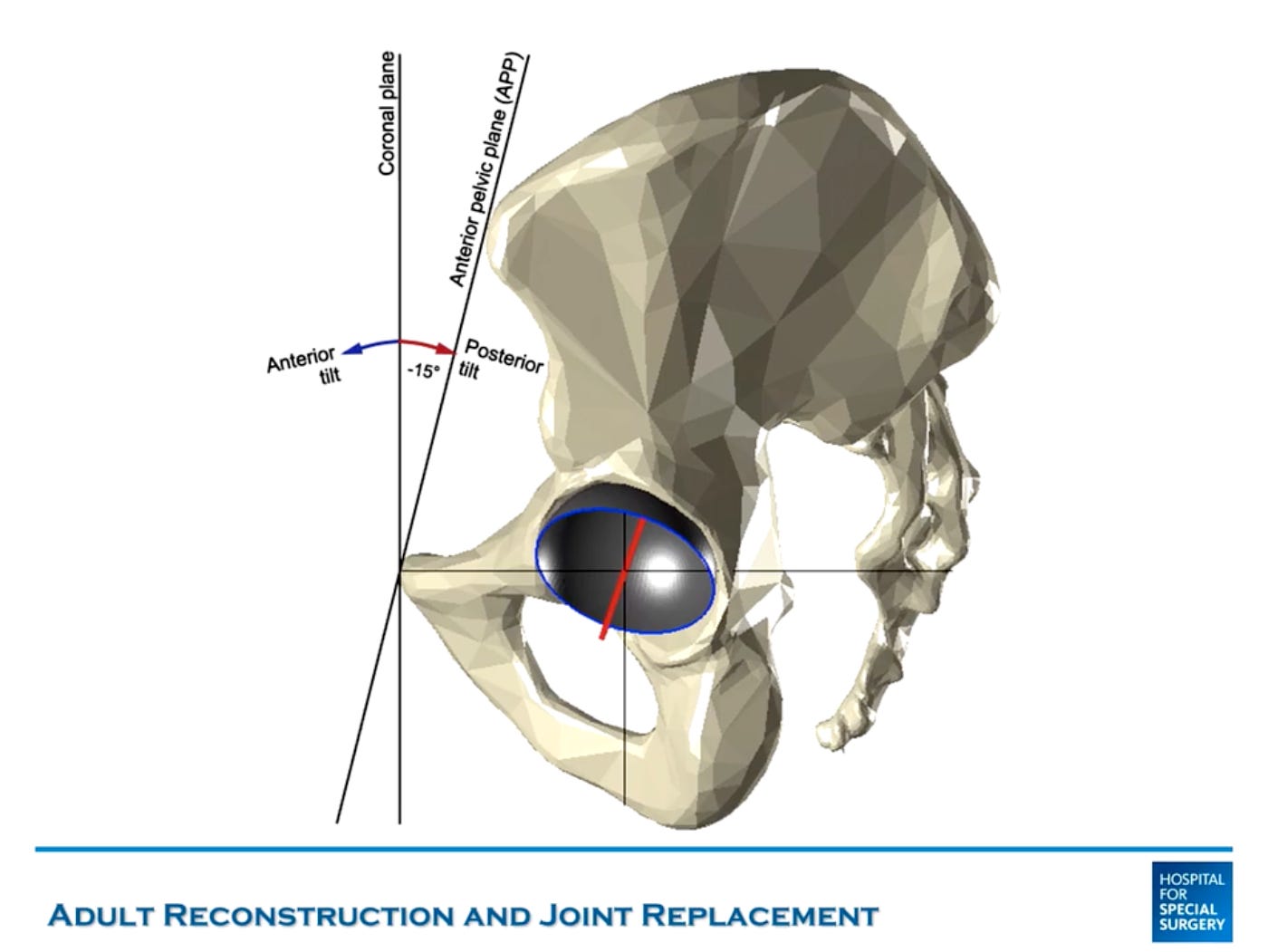
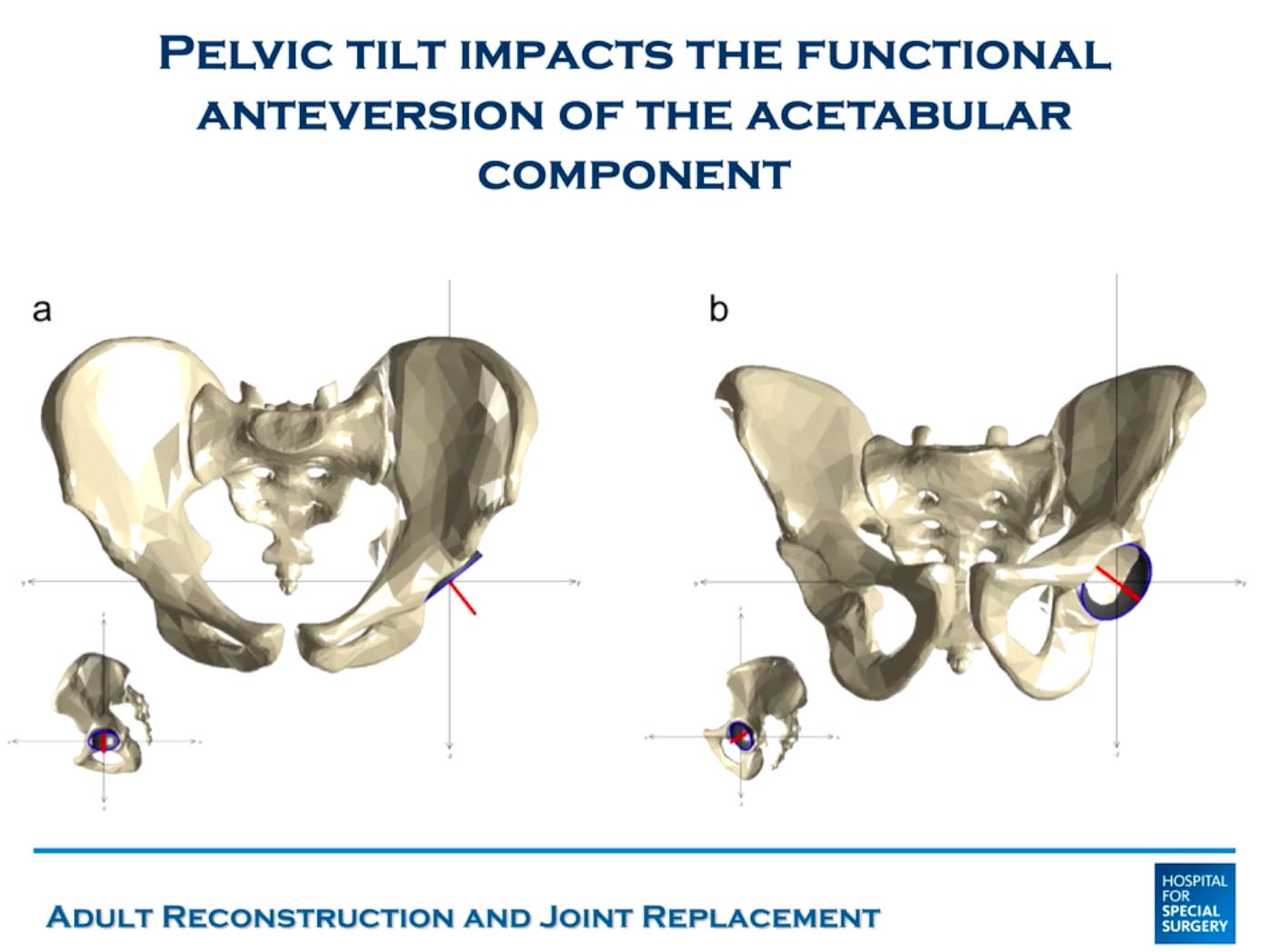
Normally, the lumbar spine is what enables this pelvic tilt. It loses lordosis (straightens) as a patient sits down. However, in stiff spines, there is less or no posterior rollback when sitting down.
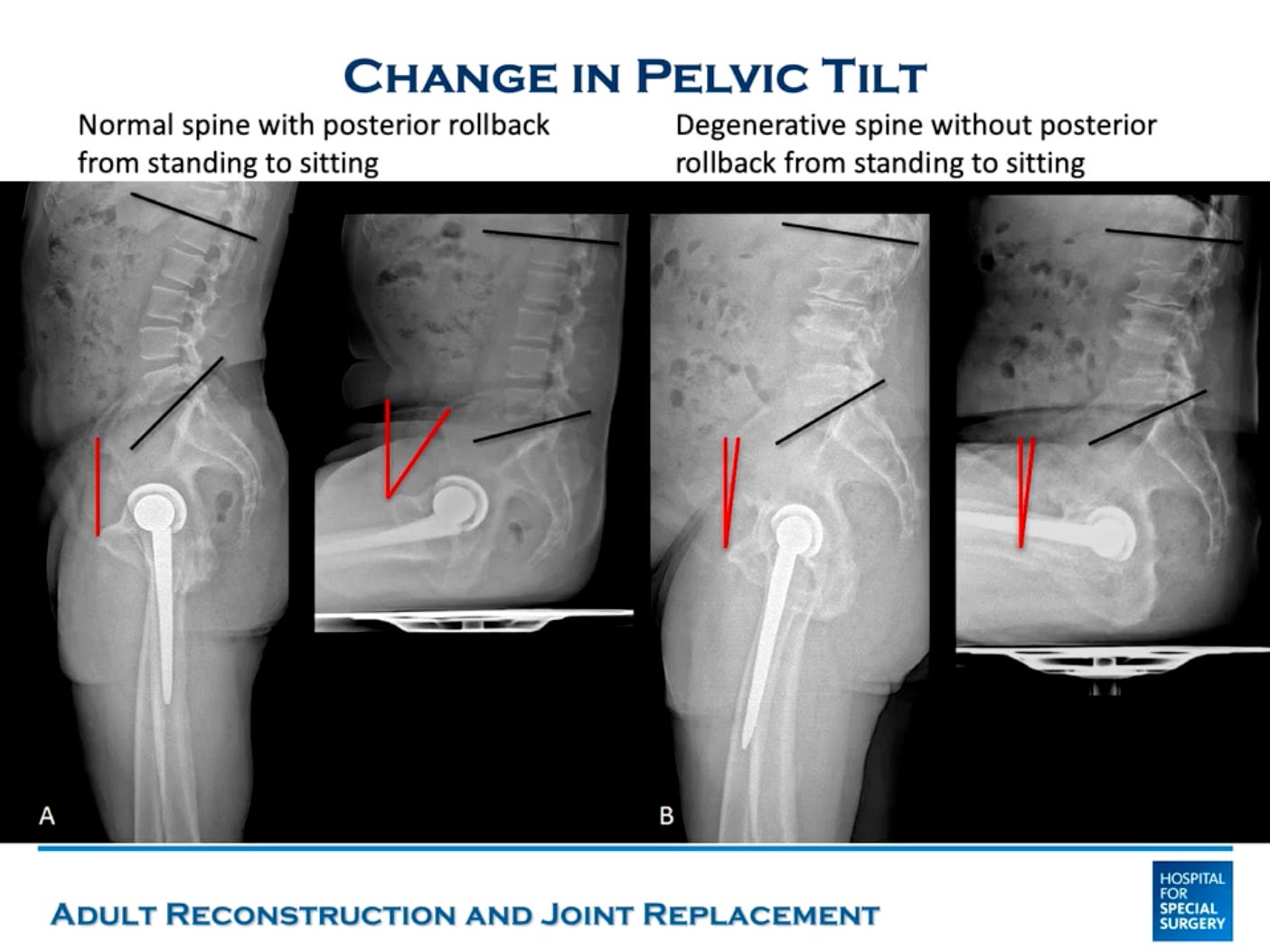
Degenerative disc disease (DDD), DDD plus scoliosis, and fusion are some of the pathologies which can lead to decreased pelvic rollback.
To compensate for this loss of pelvic rollback, and to allow the patient to still sit their butt down, more motion is required through the hip joint. Here is some data to prove it:
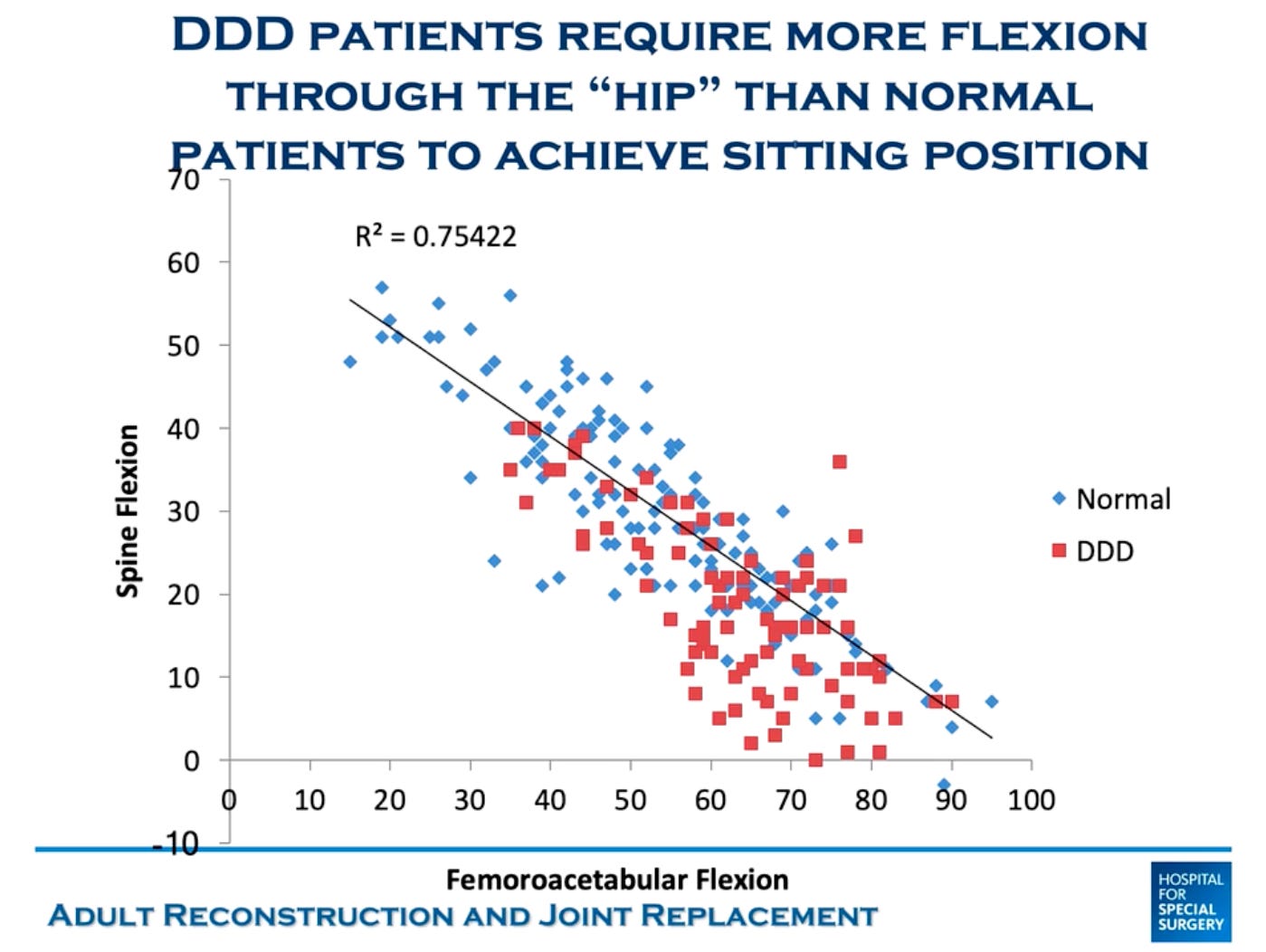
As a reminder, forcing the femoral component to move through that larger arc of motion is going to lead to higher rates of impingement at the extremes of motion. And then that impingement leads to an increased risk of dislocations.
See, it all came full circle. Also, there are some good animations in the video if that didn’t make sense. Tomorrow, we press on!
Sources
Jerabek S. How to Define the Spine-Pelvic Relationship? Are Patients with Spine Fusions at a Higher Risk of Hip Dislocations? 5TH ANNUAL TECHNOLOGY AND INNOVATION IN ORTHOPEDICS SYMPOSIUM. 2020 Feb 13. On VuMedi.
Thank you, Andrew, for recommending this.
Esposito CI, Gladnick BP, Lee YY, Lyman S, Wright TM, Mayman DJ, Padgett DE. Cup position alone does not predict risk of dislocation after hip arthroplasty. J Arthroplasty. 2015 Jan;30(1):109-13. doi: 10.1016/j.arth.2014.07.009. Epub 2014 Jul 11. PMID: 25249516; PMCID: PMC4270833.
Abdel MP, von Roth P, Jennings MT, Hanssen AD, Pagnano MW. What Safe Zone? The Vast Majority of Dislocated THAs Are Within the Lewinnek Safe Zone for Acetabular Component Position. Clin Orthop Relat Res. 2016 Feb;474(2):386-91. doi: 10.1007/s11999-015-4432-5. PMID: 26150264; PMCID: PMC4709312.

