Shout out to my coresident Kara for the inspiration on this one. I think every med student knows about ankylosing spondylitis (AS), and diffuse idiopathic skeletal hyperostosis (DISH) is pretty recognizable to me as well. But I didn’t know much about ossification of the posterior longitudinal ligament (OPLL).
What I learned today
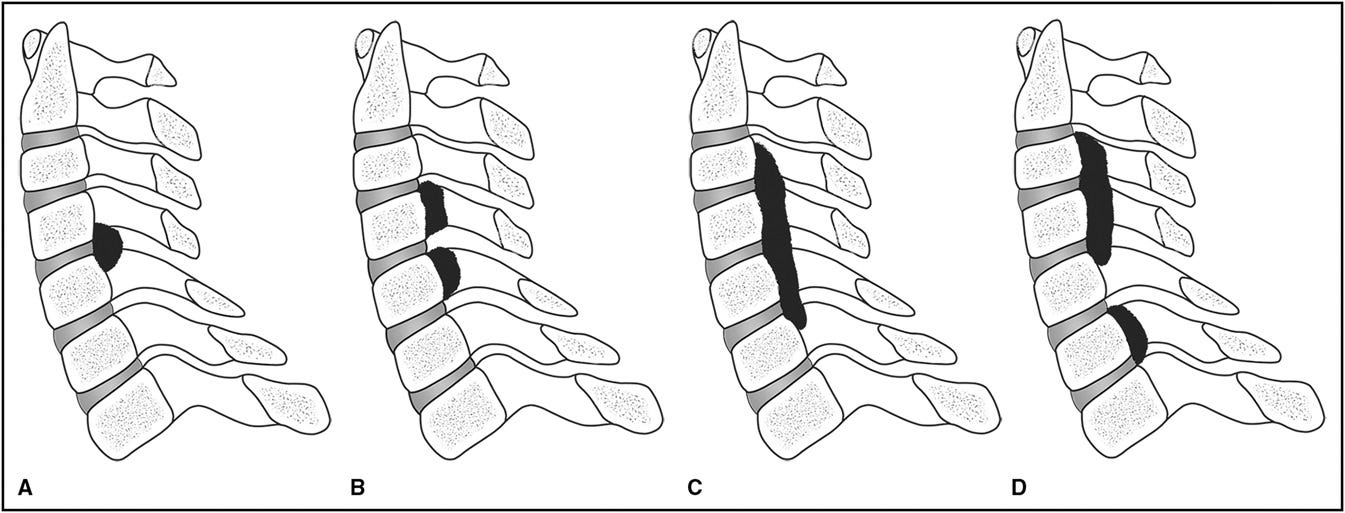
Unlike the diffuse nature of DISH and AS, OPLL mainly affects the ligament that runs along the posterior aspect of the vertebral bodies.
Pathogenesis
Chondroblast- and fibroblast-like spindle cell proliferation + vascular infiltration
PLL degeneration and hypertrophy
Endochondral ossification into mature lamellar bone
Multiple genes have been implicated, with the disease showing a genetic predisposition. The reported incidence is highest among East Asian communities (1.9-4.3%), although more recent studies have shown that roughly 0.1-1.7% of Caucasians are affected. Among Caucasians with OPLL, up to 50% have DISH as well.
Other risk factors include hypoparathyroidism, hypophosphatemic rickets, hyperinsulinemia, and obesity.
Natural history
Most frequently affects the cervical spine
2:1 male:female ratio
Roughly 1/3 meet the criteria for myelopathy at the time of OPLL diagnosis
Initial neurologic status is the best predictor for clinical progression
Risk factors for development of myelopathy: >60% spinal canal stenosis, ≤6 mm of space for cord, increased cervical ROM, and OPLL that is laterally deviated in the spinal canal
Workup
Assess for standard sx of myelopathy and perform a thorough spine exam.
Obtain sitting or standing XR to assess cervical lordosis. Kyphosis line (K-line) = drawn from center of canal at C2 to center of canal at C7. If the OPLL protrudes posterior to the K-line, this is a negative prognostic factor for posterior surgery alone.
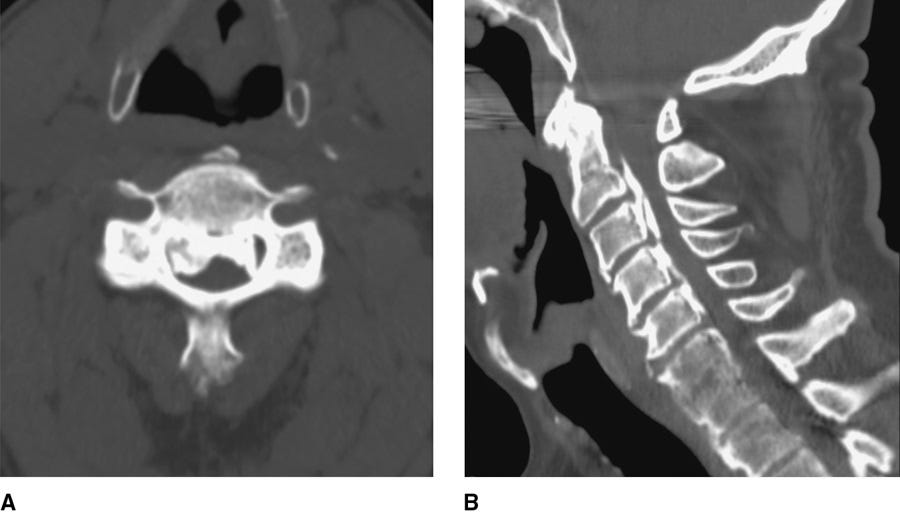
→ What is the “double-layer” sign and what does it indicate?
Dural ossification can be seen on CT as a distinct ossified band. With anterior decompression, dural tear rates are >50% with a (+) sign and 13% when absent.
On MRI, look for cord atrophy or T2 hyperintensity, which likely indicate worse outcomes even after decompression. In an acute injury, intraparenchymal edema or hematoma may be seen.
Tomorrow it gets even better… treatment~~~*!
Sources
An HS, Al-Shihabi L, Kurd M. Surgical treatment for ossification of the posterior longitudinal ligament in the cervical spine. J Am Acad Orthop Surg. 2014 Jul;22(7):420-9. doi: 10.5435/JAAOS-22-07-420. PMID: 24966248.